From Lab to Clinic : The Regulatory Journey of Medical Device Innovation
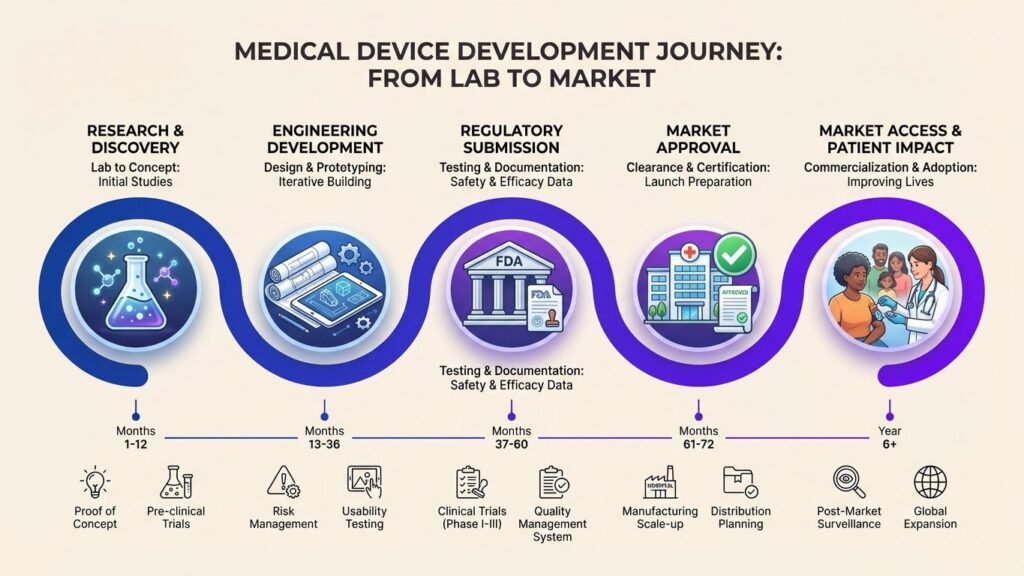
The Innovation Paradox
A breakthrough medical device sits in a laboratory. Clinical data suggests it could transform patient care. Engineers have perfected the design. Manufacturing processes are robust. Yet it remains years away from helping patients. Why?
The answer lies in a complex regulatory framework designed to ensure that medical devices reaching patients are safe, effective, and manufactured to consistent quality standards. While this process can seem daunting—particularly for innovative startups and academic researchers—understanding the regulatory pathway is essential for successfully bringing medical innovations to market.
In 2025, the FDA continues to balance two critical mandates: protecting public health through rigorous review while facilitating timely access to innovations that address unmet medical needs. For companies developing next-generation antimicrobial devices and therapies, navigating this landscape requires strategic planning, quality-focused execution, and often, patience.
Understanding Device Classification: The Foundation
The FDA’s regulatory requirements for medical devices are risk-based. Every medical device falls into one of three classes, determining the level of regulatory control required:
Class I Devices: Lowest Risk These devices pose minimal risk to users. Examples include elastic bandages, examination gloves, and hand-held surgical instruments. Most Class I devices are exempt from premarket review, requiring only registration and listing with the FDA.
Class II Devices: Moderate Risk These devices require greater regulatory control to ensure safety and effectiveness. Most antimicrobial wound care products fall into this category. Class II devices typically require 510(k) premarket notification demonstrating “substantial equivalence” to a legally marketed device.
Class III Devices: Highest Risk These devices support or sustain human life, are implanted, or present significant risk of illness or injury. Examples include heart valves, implantable pacemakers, and some high-risk drug-device combinations. Class III devices require premarket approval (PMA), the most stringent regulatory pathway.
Understanding your device’s classification is the critical first decision point that impacts development strategy, timeline, and costs.
The 510(k) Pathway: Demonstrating Substantial Equivalence
For many antimicrobial medical devices, the 510(k) pathway represents the most efficient route to market. Under the Medical Device User Fee Amendments (MDUFA) V, the FDA aims to clear 95% of 510(k) submissions within 90 FDA days.
What is Substantial Equivalence?
A device is substantially equivalent to a predicate device if it:
- Has the same intended use as the predicate
- Has the same technological characteristics, OR
- Has different technological characteristics but doesn’t raise new safety or effectiveness questions and demonstrates equivalent performance
Building a Strong 510(k) Submission
Success in the 510(k) pathway requires:
- Predicate Device Selection Identifying appropriate predicates—legally marketed devices that share similar characteristics—is crucial. The FDA’s Product Classification Database helps identify potential predicates, but strategic selection requires understanding both your device’s unique features and regulatory precedents.
- Performance Testing Demonstrating substantial equivalence typically requires:
- Bench testing showing comparable performance characteristics
- Biocompatibility testing per ISO 10993 standards
- Sterilization validation (if applicable)
- Shelf life and stability studies
- Antimicrobial efficacy testing per established protocols
- Clinical Data While not always required for 510(k)s, clinical data strengthens submissions when:
- Performance testing alone cannot demonstrate substantial equivalence
- The device incorporates new technological characteristics
- Predicate devices have limited clinical data
- The FDA requests additional evidence during review
- Labeling and Instructions for Use Clear, accurate labeling is essential. It must:
- State intended use and indications for use
- Provide adequate directions for use
- Include warnings about potential risks
- Not make unsupported claims
Common 510(k) Pitfalls to Avoid
As noted in 2025 regulatory guidance, frequent issues include:
- Inadequate predicate analysis
- Insufficient performance testing
- Poor quality of data presentation
- Inadequate risk analysis
- Labeling issues or unsupported claims
The PMA Pathway: When Innovation Requires More
For truly novel devices or those presenting significant risk, the PMA pathway provides a mechanism for FDA approval based on scientific evidence that the device is safe and effective for its intended use.
PMA Requirements
A PMA application includes:
- Complete device description and specifications
- Comprehensive nonclinical testing data
- Clinical trial data from well-controlled studies
- Manufacturing and quality system information
- Proposed labeling
- Bibliography of relevant scientific literature
PMA Timeline
Under current FDA performance goals, PMA average total time to decision approximates 285 days, though complex devices may require longer review periods.
The Critical Role of Quality Systems
Regardless of regulatory pathway, robust quality management systems (QMS) form the foundation of successful device development. The FDA’s Quality System Regulation (21 CFR Part 820) requires manufacturers to have comprehensive systems covering:
Design Controls
- Design planning and input requirements
- Design reviews at appropriate stages
- Design verification and validation
- Design transfer procedures
- Design changes management
Manufacturing Controls
- Process validation
- Equipment maintenance and calibration
- Environmental monitoring (where applicable)
- Process monitoring and control
Documentation and Record Keeping
- Device master records
- Device history records
- Quality system procedures
- Complaint files and CAPA (Corrective and Preventive Action) records
Building quality systems early—during development, not after—dramatically increases regulatory success rates and reduces costly remediation later.
The Power of Pre-Submission: Q-Submissions
One of the most valuable yet underutilized tools for device developers is the FDA’s Q-Submission program. This mechanism allows companies to obtain FDA feedback before formal submission.
Q-Submission Types Include:
- Pre-Submission meetings to discuss regulatory strategy
- Requests for feedback on testing protocols
- Information meetings about new technologies
- Determination meetings for device classification
According to 2025 regulatory data, companies using pre-submissions strategically achieve significantly higher first-pass approval rates and shorter review times.
Timing is Critical
Engage FDA early—ideally when you’ve characterized your device and planned initial testing but before generating all data. This timing allows incorporation of FDA feedback without costly redoing of studies.
Accelerated Pathways: Breakthrough Devices Program
For devices offering significant advantages over existing treatments for life-threatening or irreversibly debilitating conditions, the FDA’s Breakthrough Devices Program provides expedited development and review.
Program Benefits Include:
- Priority review
- Interactive communication with FDA reviewers
- Senior management involvement in review
- Assignment of dedicated FDA staff
- Potential for abbreviated clinical pathways
Recent analysis shows Breakthrough designation can reduce time to market by 6-12 months for qualifying devices.
The Global Perspective: CE Mark and Beyond
While FDA approval enables U.S. market access, global commercialization requires navigating additional regulatory frameworks:
European Union: CE Mark Under the Medical Device Regulation (MDR), devices must:
- Undergo conformity assessment by Notified Bodies
- Meet essential safety and performance requirements
- Maintain technical documentation
- Implement post-market surveillance systems
Other Key Markets
- Japan: PMDA approval required
- China: NMPA registration mandatory
- Canada: Health Canada licensing
- Australia: TGA registration
Strategic regulatory planning addresses multiple markets simultaneously, maximizing return on development investment.
The Post-Market Reality: Obligations Don’t End at Approval
FDA approval or clearance marks the beginning, not the end, of regulatory obligations:
Post-Market Surveillance
- Medical Device Reporting (MDR) of adverse events
- Correction and removal reporting
- Annual registration and listing updates
- Unique Device Identification (UDI) implementation
Quality System Inspections FDA conducts inspections of device manufacturers to verify QMS compliance. Preparation for inspections should be continuous, not triggered by inspection announcement.
Post-Market Studies In some cases, FDA requires post-approval studies to gather additional real-world evidence about device performance, particularly for novel technologies or those approved through accelerated pathways.
Real-World Example: Our Journey
Our experience developing FDA-cleared antimicrobial wound care devices illustrates these principles in practice:
Phase 1: Foundation Building (Year 1)
- Established GMP-compliant manufacturing facility
- Built comprehensive quality management system
- Conducted extensive preclinical testing
- Identified appropriate predicates
Phase 2: Regulatory Preparation (Year 2)
- Held FDA pre-submission meetings
- Refined testing protocols based on FDA feedback
- Completed biocompatibility and performance testing
- Prepared comprehensive 510(k) submissions
Phase 3: FDA Review and Approval (Year 2-3)
- Submitted 510(k) applications
- Responded to FDA questions and requests
- Achieved 510(k) clearance for multiple indications
- Obtained FDA establishment registration
Phase 4: International Expansion (Year 3-4)
- Secured CE Mark certification
- Established European distribution partnerships
- Implemented post-market surveillance systems
- Continued innovation pipeline development
This journey required significant investment, careful planning, and unwavering commitment to quality—but resulted in cleared medical devices now benefiting patients globally.
Lessons Learned: Success Factors
Through this experience, several success factors emerged:
1. Quality from Day One Building quality systems early prevents costly remediation and delays. Quality isn’t something added at the end; it’s fundamental from the beginning.
2. FDA Engagement Viewing FDA as a partner, not adversary, through early engagement and transparent communication dramatically improves outcomes.
3. Scientific Rigor Robust testing and clear documentation of results builds FDA confidence and accelerates review.
4. Expert Guidance Engaging regulatory consultants with device-specific expertise helps navigate complex requirements and avoid common pitfalls.
5. Resource Planning Regulatory processes require significant resources—human, financial, and time. Realistic planning prevents mid-process resource crises.
The Cost of Innovation: Investment Required
Regulatory compliance and clinical development require substantial investment:
Typical 510(k) Program Costs:
- Testing and data generation: $100,000-300,000
- Regulatory submission preparation: $30,000-100,000
- FDA filing fees: ~$13,000 (2025 rates)
- Quality system implementation: $50,000-200,000
PMA Program Costs:
- Significantly higher, often $2-10+ million
- Clinical trials represent major cost driver
- Extended timelines increase burn rate
Post-Market Costs:
- Quality system maintenance: $100,000+/year
- Post-market surveillance: $50,000+/year
- Regulatory updates and modifications: Variable
These figures underscore why many academic innovations fail to reach commercialization—the “valley of death” between proof of concept and marketed product.
Looking Forward: Evolving Regulatory Landscape
The regulatory environment continues to evolve:
Increasing Digital Integration FDA is embracing artificial intelligence and digital health technologies, creating new pathways for algorithm-based devices and connected systems.
Real-World Evidence The FDA increasingly accepts real-world evidence from routine clinical practice to supplement traditional clinical trials, particularly for post-market safety monitoring.
Streamlined Pathways New initiatives like the Commissioner’s National Priority Voucher program (launched 2025) offer accelerated review for devices addressing critical national needs, including antimicrobial resistance.
Global Harmonization Efforts toward international standards harmonization through organizations like IMDRF (International Medical Device Regulators Forum) aim to reduce duplicative requirements across markets.
Conclusion: The Long View
The regulatory journey from laboratory innovation to approved medical device is long, complex, and demanding. It requires substantial investment, unwavering commitment to quality, strategic thinking, and often, patience that tests even the most dedicated developers.
Yet this rigorous process serves a critical purpose: ensuring that devices reaching patients are safe, effective, and manufactured to consistent standards. Every cleared or approved device represents validation that the innovation will genuinely benefit patients without causing unacceptable risk.
For companies developing antimicrobial innovations—whether devices, drug-device combinations, or novel therapies—understanding and embracing the regulatory pathway is essential. Success requires viewing regulatory compliance not as a hurdle to overcome but as a framework ensuring your innovation truly delivers on its promise to improve patient care.
The journey is challenging, but for innovations that address unmet medical needs, improve patient outcomes, and advance the standard of care, it’s a journey worth taking. With careful planning, quality-focused execution, and strategic regulatory approach, transformative medical devices can successfully navigate from laboratory concept to clinical reality.
And that’s when innovation truly matters—when it reaches the patients who need it most.
