Beyond Antibiotics : How HOCl-Based Solutions Combat Antimicrobial Resistance
The Growing Crisis: When Antibiotics Stop Working
In 2025, antimicrobial resistance (AMR) has emerged as one of the most pressing threats to global health. The World Health Organization warns that drug-resistant infections could claim more lives than cancer by 2050 if current trends continue. Every time a doctor prescribes antibiotics, every time a patient fails to complete their antibiotic course, every time antibiotics are used unnecessarily, resistant bacteria gain an evolutionary advantage.
The statistics are sobering: Infections caused by antimicrobial-resistant pathogens now contribute to approximately 1.27 million deaths globally each year. Methicillin-resistant Staphylococcus aureus (MRSA), vancomycin-resistant Enterococcus (VRE), and multi-drug resistant Pseudomonas aeruginosa are no longer hospital curiosities—they’re everyday challenges in clinical practice.
But what if there was an antimicrobial agent that bacteria have been exposed to for millions of years yet have never developed meaningful resistance against? Enter hypochlorous acid (HOCl), a molecule your own immune system produces to fight infections.
HOCl: Nature’s Original Antimicrobial
Hypochlorous acid isn’t a laboratory invention—it’s biology’s answer to microbial threats. When your body detects an infection, neutrophils (white blood cells) rush to the site and produce HOCl through an enzyme called myeloperoxidase. In fact, approximately 70% of hydrogen peroxide produced by neutrophils is converted into HOCl. This powerful oxidant is your immune system’s first line of defense against invading pathogens.
Consider this remarkable fact: An estimated 10⁶ stimulated neutrophils can produce approximately 0.2 μmol of HOCl during a 2-hour period. That tiny amount is enough to destroy 150 million E. coli cells in milliseconds. This extraordinary potency, combined with its rapid action and natural occurrence in the body, makes HOCl fundamentally different from synthetic antibiotics.
How HOCl Works: A Multi-Target Approach
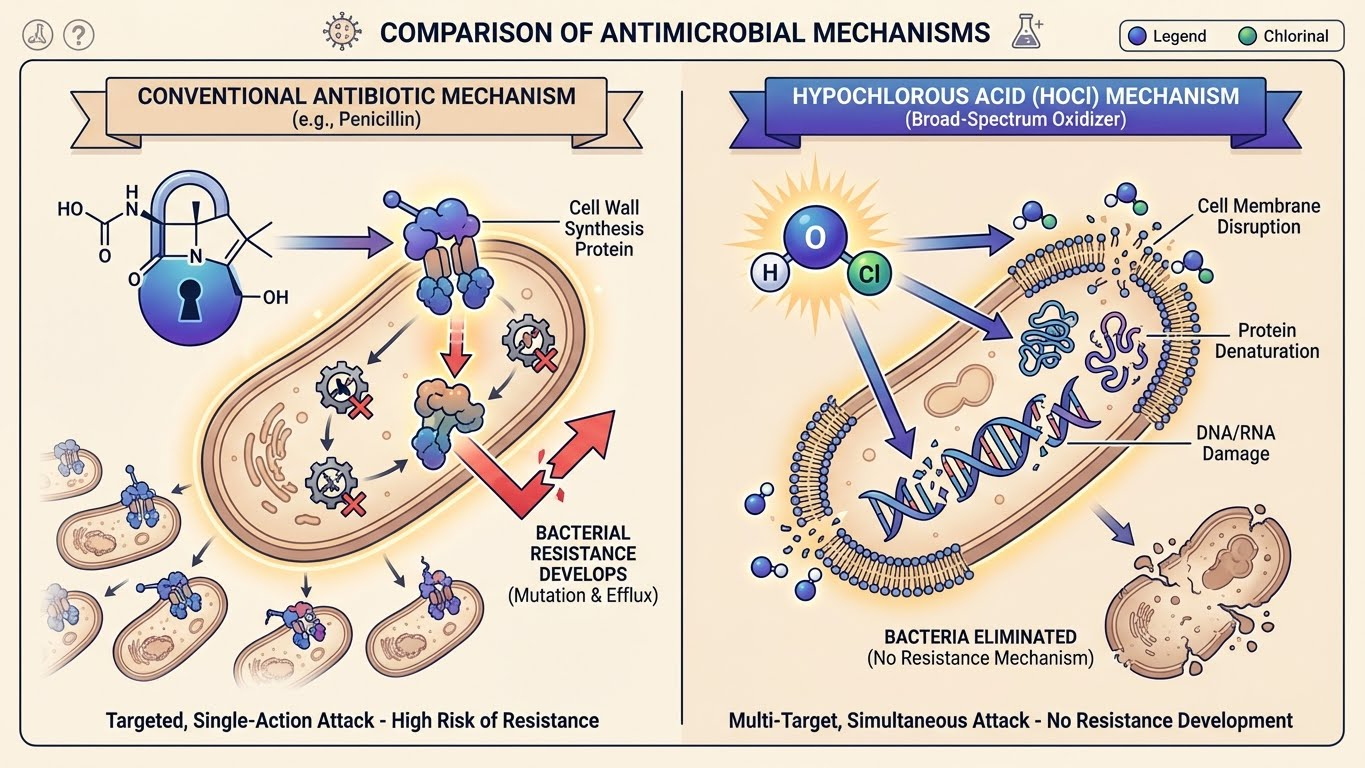
Unlike antibiotics, which typically target specific bacterial structures or processes (like cell wall synthesis or protein production), HOCl operates through a multi-faceted mechanism that makes resistance development extraordinarily difficult.
Multiple Cellular Targets
HOCl interacts with several biomolecules simultaneously:
- Sulfur-Containing Amino Acids: HOCl rapidly reacts with cysteine and methionine residues in proteins, causing protein denaturation and loss of function
- Lipid Membranes: It disrupts both the outer and inner bacterial membranes, causing leakage of cellular contents and cell death
- Nucleic Acids: HOCl damages DNA and RNA, preventing bacterial replication and protein synthesis
- Membrane Components: It targets lipopolysaccharides in Gram-negative bacteria and peptidoglycan in Gram-positive bacteria
This multi-pronged attack means bacteria would need to simultaneously develop multiple resistance mechanisms—a virtually impossible evolutionary feat. As one researcher noted, it would be like trying to defend a castle when attackers are breaching the walls, the gates, the moat, and tunneling from below all at once.
The Speed Advantage
HOCl’s antimicrobial action occurs within seconds. Recent studies demonstrate that stabilized HOCl solutions kill bacteria within the first minute of contact, with accurate killing times as short as 12 seconds. This rapid action prevents bacteria from activating stress response mechanisms or initiating resistance gene expression.
The Resistance Question: Why HOCl Succeeds Where Antibiotics Fail
The fundamental difference between HOCl and conventional antibiotics lies in their mechanisms of action and bacteria’s ability to adapt.
Antibiotic Resistance Mechanisms
Bacteria develop antibiotic resistance through several well-characterized mechanisms:
- Producing enzymes that destroy the antibiotic (like beta-lactamases)
- Modifying the antibiotic’s target site
- Reducing antibiotic uptake through membrane changes
- Actively pumping antibiotics out of the cell (efflux pumps)
- Developing alternative metabolic pathways
HOCl Resistance: Theoretical But Rare
While research has identified some bacterial defense mechanisms specific to HOCl stress—including three transcriptional regulators (HypT, RclR, and NemR) and four chaperone holdases (Hsp33, RidA, Cnox, and polyP)—these provide only limited protection.
Critically, these mechanisms don’t prevent HOCl from killing bacteria; they merely help some cells survive sub-lethal exposure. Even bacteria with these defense systems activated remain susceptible to therapeutically relevant HOCl concentrations.
Some studies have shown that certain bacteria can adapt to low levels of sodium hypochlorite (bleach) under specific laboratory conditions. However, as noted in 2025 research, such resistance is “infrequent” and has not been observed clinically with properly formulated HOCl solutions used at appropriate concentrations.
The Biofilm Advantage
One of HOCl’s most significant advantages emerges in the context of biofilms—those bacterial fortresses that render conventional antibiotics largely ineffective.
Research published in 2025 demonstrates that stabilized HOCl solutions maintain antimicrobial activity within biofilms at dilutions ranging from 1/32 to 1/16. More impressively, the concentration needed to kill bacteria within biofilms is the same as that needed to prevent biofilm formation—a stark contrast to antibiotics, which typically require 100-1,000 times higher concentrations to achieve biofilm penetration.
HOCl achieves this through several mechanisms:
- Physical disruption of the extracellular polymeric substance (EPS) matrix
- Rapid oxidation of biofilm components
- Penetration capabilities that don’t rely on specific transport mechanisms
- Action against dormant persister cells that antibiotics miss
Clinical Applications: From Wounds to Respiratory Infections
The unique properties of HOCl have led to expanding clinical applications:
Wound Care FDA-cleared HOCl solutions are revolutionizing chronic wound management. A 2025 study showed that HOCl’s rapid antimicrobial action combined with wound healing enhancement properties makes it ideal for treating infected wounds without the risk of resistance development.
Respiratory Applications Recent research exploring HOCl for respiratory infections shows promising results. As a 2025 article in Viruses notes, HOCl’s successful history in wound treatment, combined with low cytotoxicity and documented efficacy against respiratory pathogens (including influenza and SARS-CoV-2), suggests significant potential for inhalation therapy.
Surgical Site Preparation HOCl solutions are increasingly used for pre-operative skin antisepsis. Studies demonstrate significant bacterial load reduction without altering microbial diversity—avoiding the risk of opportunistic infections that can occur with broad-spectrum antibiotics.
Environmental Disinfection Healthcare facilities are adopting HOCl for surface disinfection, particularly in areas requiring frequent cleaning where traditional disinfectants pose toxicity concerns or leave harmful residues.
The Stability Challenge: Not All HOCl Is Equal
Traditional HOCl solutions face a significant limitation: instability. Conventional production methods create HOCl that degrades rapidly (within 90 days) and loses efficacy in the presence of organic matter—precisely the conditions found in clinical use.
This limitation has historically prevented HOCl from achieving its full therapeutic potential. However, recent advances in stabilization technology have produced HOCl formulations that:
- Maintain stability for extended periods
- Retain antimicrobial efficacy in the presence of blood serum
- Remain effective at high dilutions with wound exudate
- Demonstrate freeze-stability for global distribution
These next-generation HOCl solutions represent a paradigm shift in antimicrobial therapy.
Safety Profile: Gentle Yet Powerful
One of HOCl’s most remarkable characteristics is its safety profile. Unlike many antimicrobial agents that demonstrate toxicity concerns, HOCl is:
Non-Toxic to Human Cells Because HOCl is naturally produced by the body, human cells have evolved mechanisms to handle it. At therapeutic concentrations, HOCl solutions don’t damage healthy tissue.
Promotes Wound Healing Research demonstrates that HOCl has dose-dependent favorable effects on fibroblast and keratinocyte migration—the cells responsible for wound closure. This means HOCl doesn’t just kill bacteria; it actively supports healing.
No Systemic Absorption When used topically, HOCl doesn’t enter the bloodstream in therapeutically significant amounts, eliminating concerns about systemic toxicity or interactions with other medications.
Environmental Safety HOCl breaks down into water and salt, creating no harmful environmental residues—a stark contrast to many conventional disinfectants.
The Economic Argument
Beyond clinical benefits, HOCl offers economic advantages:
- Reduced need for expensive antibiotics
- Shorter treatment durations due to rapid action
- Lower rates of resistance-related treatment failures
- Decreased hospital stays for infection management
- Reduced environmental remediation costs
As healthcare systems worldwide face budget constraints while antimicrobial resistance drives costs upward, HOCl represents a cost-effective alternative that doesn’t compromise efficacy.
Looking Forward: A Complementary Approach
HOCl isn’t intended to replace antibiotics entirely—that would be neither practical nor desirable. Instead, it represents a powerful complementary tool in the infection control arsenal:
- First-Line Topical Treatment: For wound infections and skin antisepsis where direct application is possible
- Biofilm Management: Where antibiotics show limited efficacy
- Environmental Control: Reducing pathogen load in healthcare settings
- Antibiotic Stewardship: Reserving antibiotics for systemic infections where they’re truly necessary
This strategic approach—using HOCl for topical and environmental applications while reserving antibiotics for systemic infections—represents smart antimicrobial stewardship.
The Role of Innovation
The future of HOCl in clinical practice depends on continued innovation:
- Improved stabilization technologies
- Formulations optimized for specific applications
- Combination approaches that synergize HOCl with other modalities
- Delivery systems that maximize efficacy while minimizing waste
Research into these areas continues to advance, with promising results emerging regularly.
Conclusion: A Natural Solution for a Modern Problem
Antimicrobial resistance represents one of healthcare’s greatest challenges, but HOCl offers a scientifically sound, clinically proven alternative that works with the body’s natural defenses rather than against them.
As we face a future where conventional antibiotics become increasingly ineffective, solutions rooted in nature’s own antimicrobial strategies become not just valuable—they become essential. HOCl’s unique combination of potent antimicrobial action, minimal resistance risk, excellent safety profile, and support for wound healing positions it as a cornerstone of 21st-century infection control.
For healthcare providers seeking to combat infection while preserving the effectiveness of our remaining antibiotics, HOCl-based solutions represent a promising path forward—one that’s been proven effective over millions of years of evolution.
